Desmoplastic melanoma is a rare, fibrosing variant of vertical growth phase spindle cell melanoma, first described in 1971 by Conley and coworkers. This subtype of melanoma presents as a light-colored, slightly raised, indurated lesion that develops more frequently in chronically sun-damaged areas in people with skin phototype I. Where pigmentation is present, it is unevenly distributed .
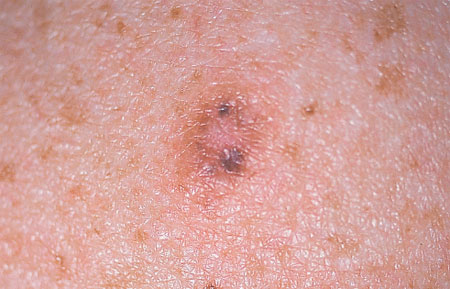
The predilection sites for desmoplastic melanoma include the head, neck and upper back, although rare cases have been reported with mucosal or acral localization. The disease has a peak incidence between the ages of 60 and 80.
Histologically, desmoplastic melanoma can mimic some melanocytic nevi and show neuroma-like histological features. Tumor cells are often spindle-shaped, hyperchromatic and distributed singly or in bundles or nests among the collagen fibers of the papillary and reticular dermis. Mitotic figures are rare and there is a constant presence of nodular lymphocytic infiltrates, while macrophages are present throughout the lesion.
Tumor cell immunoreactivity is strongly positive for S100 protein, but often negative for other markers, such as tyrosinase, gp100, Melan A, HMB45, NKI/beteb, and Leu 7 (CD57). In a small percentage of cases, the tumor cells are labeled with CD68.
Because of its nonspecific clinical features, the diagnosis of desmoplastic melanoma is often delayed, when the tumor has already infiltrated the reticular dermis. In these stages, it can be confused with other dermatological conditions, such as a hypertrophic scar, dermatofibroma or basal cell carcinoma. Epiluminescence images show the same features as melanoma.
Although desmoplastic melanoma is associated with frequent local recurrences, probably due to its neurotropism, lymph node metastases are less frequent. This, together with its thickness according to Breslow, makes the prognosis of desmoplastic melanoma generally better than that of nondesmoplastic melanomas. A typical treatment for desmoplastic melanoma requires wide excision of the lesion.
Desmoplastic melanoma, although its clinical manifestations can be deceptive, is a tumor that requires immediate medical attention once detected. The difficulty in early diagnosis is due to the similarity of this lesion to other less serious skin conditions. Its induration, absence of ulceration and light color can make it appear less threatening than it really is.
Because of its propensity to develop in sun-exposed areas, it is of paramount importance for people with skin type I to closely monitor their skins and seek immediate medical advice for any suspicious changes. The importance of periodic skin exams by a dermatologist cannot be emphasized enough for these high-risk populations.
Although the prognosis for desmoplastic melanoma may be better than for other forms of melanoma, with lymph node metastases less common, the risk of local recurrence is significant. This tumor exhibits neurotropism, meaning it tends to grow along nerves, making management of local recurrences a significant challenge.
Treatment options for desmoplastic melanoma include wide excision of the lesion. The extent of the excision will depend on the extent of the tumor. In advanced cases, more aggressive therapies, such as immunotherapy or chemotherapy, may need to be considered. Finally, because desmoplastic melanoma can have an aggressive course and can lead to serious complications, a multidisciplinary approach to patient management is crucial.