The etiology of melanoma is multifactorial, among the most important risk factors for melanoma there is, as we have already written, exposure to excessive, intermittent ultraviolet light, mainly in childhood; moreover, among the risk factors we must consider a personal or family history of melanoma, the skin phototype, the number of melanocytic nevi, immunosuppression, multiple atypical nevi, finally giant congenital nevi, age, genetic factors.

Sun exposure
in recent years a close correlation has been noted between melanoma and excessive sun exposure, it has been seen that people with a light phototype (freckles, light hair, light eyes) had a greater incidence of melanoma, particularly in cases where these people they exposed themselves to the sun excessively and intermittently. Populations with fair skin have a frequency of melanoma 10 times higher than blacks and 7 times higher than Hispanic Americans. A personal history of sunburn before age 20 is associated with an increased risk. Studies on animals show that it is the UVB rays emitted by the sun that favor the development of melanoma, while the role of UVA is doubtful. Phototype: people with blue or green eyes, blond or red hair, freckles are at a greater risk of developing melanoma. People with light hair have a double incidence of melanoma compared to people with dark hair Giant congenital nevi: people with giant congenital nevi with a diameter greater than 15 cm have a 6% risk of developing melanoma and 50% develop it in the first 5 years of life. Such melanomas are often deep and spread into the subcutaneous tissue.
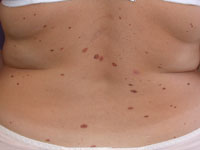
Multiple atypical nevi:
The presence of multiple atypical or dysplastic nevi is related to a high risk of developing melanoma (about 7 times higher than normal). It is believed that patients with dysplastic nevus syndrome, a family history of atypical nevi, and multiple family members with melanoma have a 100% chance of developing melanoma in their lifetime.
Storia familiare di melanoma:
A family history of melanoma increases the risk of developing melanoma 3 to 8 times. Genetic studies have identified a familial melanoma gene, CDKN2, on chromosome 9p21 that encodes a tumor suppressor protein p16.16. Mutations of this gene have been documented in 30% of patients with familial melanoma. A mutation in the CDK4 gene that alters the docking site of the p16-interacting protein with impaired cell cycle regulation. Some studies find changes in melanocortin 1 receptor (MC1R) receptor (MC1R) susceptibility to sunburn.

UV artificiali:
exposure to artificial UV rays (sunbeds) for more than 10 sessions a year increases the risk of melanoma by 2 times in people over 30 years old.
Immunosoppressione:
this factor increases the risk of developing melanoma particularly in patients with lymphoma, leukemia or organ transplants, even if the possibility of developing skin cancers is higher. The chance of developing melanoma is 2.5 times greater in people who receive a transplant or have lymphoma, and they are 2.8 times more likely to develop metastatic melanoma.

Numero dei nevi:
epidemiology studies have shown that people with numerous nevi have a higher incidence of melanomas. One study found that the number of melanoma cases was twice as high in individuals with more than 50 nevi as in people with fewer than 15 nevi. Out of 4 melanomas, one appears to be related to a pre-existing nevus.
Age:
melanoma a tumor that prevails in adults (average age around 50 years) although in recent years there has been an increase in the incidence of melanoma in adolescence and childhood
Gender:
in the United States it has a greater frequency in men, women also have a higher survival xhw passes 95 at 5 years in patients aged 15 to 29 years against 88% of men.
Ethnic factors:
l’incidenza del melanoma è correlata alla pigmentazione cutanea, quindi la massima incidenza è tra la razza caucasica e la minor incidenza nella razza negra, anche se alcune forme tumorali come il melanoma acrolentigginoso prevalgano negli ispanici
Genetic factors:
people with xeroderma pigmentosum have a higher risk than the general population of developing melanoma in exposed areas. These patients have a 1000-fold increase in the possibility of developing skin tumors (carcinoma or basal cell carcinoma) compared to the general population. This is due to a genetic defect in DNA repair for which there is a large possibility that solar radiation will induce a carcinogenic mutation. Other diseases with an increased incidence of melanomas are hereditary retinoblastoma (about 7% of these patients develop melanomas) and Li-Fraumeni syndrome, neurofibromatosis, mutations in CDKN2A and CKD4 explain some familial melanomas.